HEALTH AND FITNESS
ABPM Machine Technology in 2025: What Has Changed and Why It Matters for Clinical Practice

Ambulatory blood pressure monitoring has been a clinical tool for over four decades. In that time, the abpm machine has evolved from a bulky, research-grade instrument into a compact, validated medical device available in a wide range of form factors and price points. Many of those advances are genuinely clinically meaningful, not just marketing iterations. Understanding what has changed and what has not helped clinical staff and procurement teams make better decisions about when to upgrade, what to upgrade to, and why it matters for patient outcomes.
Table of Contents
The First Generation: Research Origins and Clinical Adoption
The first practical ambulatory blood pressure monitors were developed in the late 1970s, primarily as research instruments for investigating the relationship between blood pressure variability and cardiovascular outcomes. These early devices were heavy, recorded data on magnetic tape, and required specialized equipment to read the results. Clinical use was limited.
By the 1980s and 1990s, lighter solid-state recorders and digital readout technology had made ambulatory monitoring accessible to clinical practice. Devices of this era established the basic architecture that would persist for several decades: an Oscillo metric upper-arm cuff connected by rubber tubing to a separate recorder unit worn on a belt or in a shoulder bag.
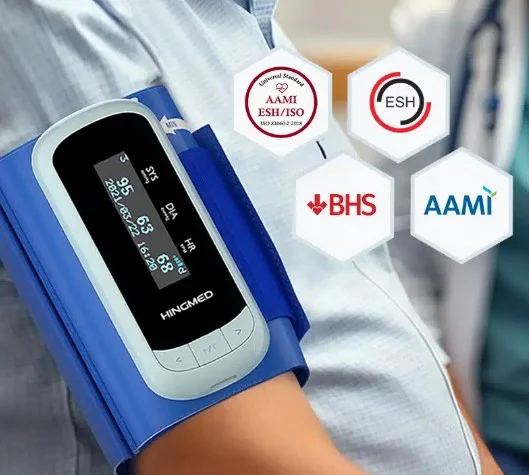
This design served clinical needs adequately for many years and accumulated the large validation dataset that underpins current guidelines. But it also had persistent drawbacks, principally related to patient comfort during sleep and the vulnerability of the rubber tube connection.
Key Advances in Modern ABPM Machines
1. Integrated All-in-One Design
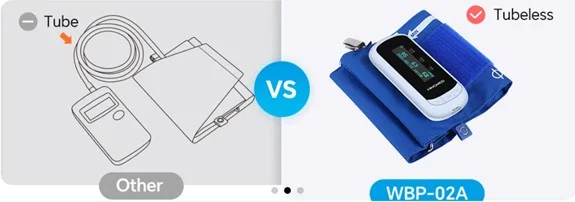
The most significant design shift of recent years has been the move toward integrating the recorder, display, pump, and battery into the cuff unit itself. This eliminates the rubber tube entirely, removing the primary source of nocturnal patient discomfort and reducing the mechanical failure point that tubing represents in high-use clinical environments.
This design approach has been adopted by several manufacturers, including hingmed, whose WBP-02A puts all functional components directly on the cuff. The result is a device that patients report as significantly less disruptive during sleep, and which tends to remain correctly positioned on the arm throughout the night, reducing artifacts caused by cuff migration.
2. Motion Artifact Filtering
Movement during cuff inflation is a major source of invalid readings in ambulatory monitoring. In older-generation devices, a patient walking upstairs or gesturing during a conversation could generate a reading that was so far from baseline as to be clinically useless, or worse, misleading. Modern ABPM machines incorporate algorithmic filters that identify and flag motion-contaminated readings, reducing the rate of erroneous inclusions in the dataset.
The sophistication of these filters varies between manufacturers and models. Some systems use accelerometer data to detect movement; others rely on waveform analysis alone. Devices with accelerometer-based filtering generally show better performance in active patients.
3. Improved Analysis Software
The hardware records the data; the software determines its clinical utility. Older ABPM software often required manual configuration of daytime and nighttime periods and produced reports that varied significantly in format and completeness. Modern platforms offer automatic period allocation based on patient diary entries, standardized report templates aligned with current guideline parameters, and export functions compatible with common EMR systems.
The best current software generates reports covering 24-hour mean values, daytime and nighttime means, dipping classification, blood pressure load, and morning surge, all within a single structured document that can be inserted directly into the patient’s electronic record.
4. Connectivity and Remote Monitoring
A more recent development is the integration of Bluetooth or USB connectivity, allowing data to be transferred from the device to a clinical workstation or cloud-based platform without manual removal of a memory card. Some newer devices support near-real-time data review, enabling clinical staff to check session progress remotely and identify technical problems before the monitoring period is complete.
When Is an Upgrade Justified?
Departments running older ABPM equipment often face a genuine question: when does the cost and disruption of upgrading become justified by clinical benefit? Several indicators suggest that existing equipment may no longer be meeting clinical needs:
- High rates of invalid readings per session, requiring repeat monitoring and increasing patient burden.
- Frequent patient complaints about overnight discomfort, leading to incomplete sessions.
- Software that does not generate reports aligned with current guideline parameters.
- Mechanical failures: tube cracks, connector failures, pump degradation requiring frequent device maintenance or removal from service.
- Inability to integrate data into the department’s current EMR system without manual workarounds.
If two or more of these apply, a structured evaluation of available alternatives is warranted.

What to Look for in a New ABPM Machine
The evaluation criteria for a new device should cover clinical validation, patient comfort, software quality, and operational durability. Specifically:
- Independent validation against a recognized protocol (BHS, AAMI/ANSI SP10, or ESH-IP).
- Patient feedback on overnight comfort, ideally from a structured trial period.
- Report template review: does the software output meet current guideline recommendations?
- EMR compatibility: can data be imported directly, or is manual data entry required?
- Cuff size range: does the device accommodate the full range of arm circumferences likely to be encountered in your patient population?
- Warranty and service terms, including calibration requirements and support response time.
The Operational Argument for Better Equipment
Beyond the clinical case, there is an operational argument for investing in modern ABPM equipment. Devices that generate more valid readings per session reduce the rate of repeat monitoring requests, which has direct resource implications. Devices with better software reduce the clinical staff time required to interpret and document results. Devices that are more comfortable reduce no-show and early-termination rates.
In a department conducting 200 or more ABPM sessions per year, even small improvements in session completion rate and data quality translate into meaningful time and cost savings over the device lifetime.
Frequently Asked Questions
How long do ABPM machines last before needing replacement?
With proper maintenance and calibration, most clinical-grade ABPM devices have an operational life of 5–8 years. Cuffs and tubing in devices that use tubing typically require replacement more frequently, often after 50–100 sessions per cuff.
How often should ABPM devices be calibrated?
Most manufacturers and quality standards recommend annual calibration checks. Some high-volume departments calibrate more frequently, particularly if devices are shared across multiple clinical sites or used in research contexts where measurement precision is more critical.
Is there a meaningful difference between ABPM machines from different manufacturers?
Yes, particularly in areas of patient comfort, motion artifact handling, and software quality. Validation status is broadly comparable among reputable manufacturers, but practical performance in clinical use can differ significantly. Requesting a trial period before committing to a purchase is the best way to evaluate real-world differences.
Conclusion
The abpm machine has come a long way from its research-grade origins. Today’s best devices offer a combination of clinical accuracy, patient comfort, and software integration that earlier generations could not match. For departments still running equipment that predates these advances, the case for evaluating alternatives is genuinely compelling not as an exercise in adopting new technology for its own sake, but because better monitoring equipment produces better data, and better data underpins better clinical decisions.
-

 GENERAL10 months ago
GENERAL10 months agoChristofle – For Those Who Dream of Family Heirloom Silver
-

 SPORTS12 months ago
SPORTS12 months agoDiscover the World of Football with Streameast: Watch Your Favorite Leagues and Tournaments
-

 GENERAL4 months ago
GENERAL4 months agoUncovering the World of кинокрадко: The Dark Side of Film Piracy
-

 GENERAL3 weeks ago
GENERAL3 weeks agoATFBooru: Anime, Gaming, and Subculture Imageboard


























