HEALTH AND FITNESS
Sleep Apnea: Possible Causes and Treatment Options
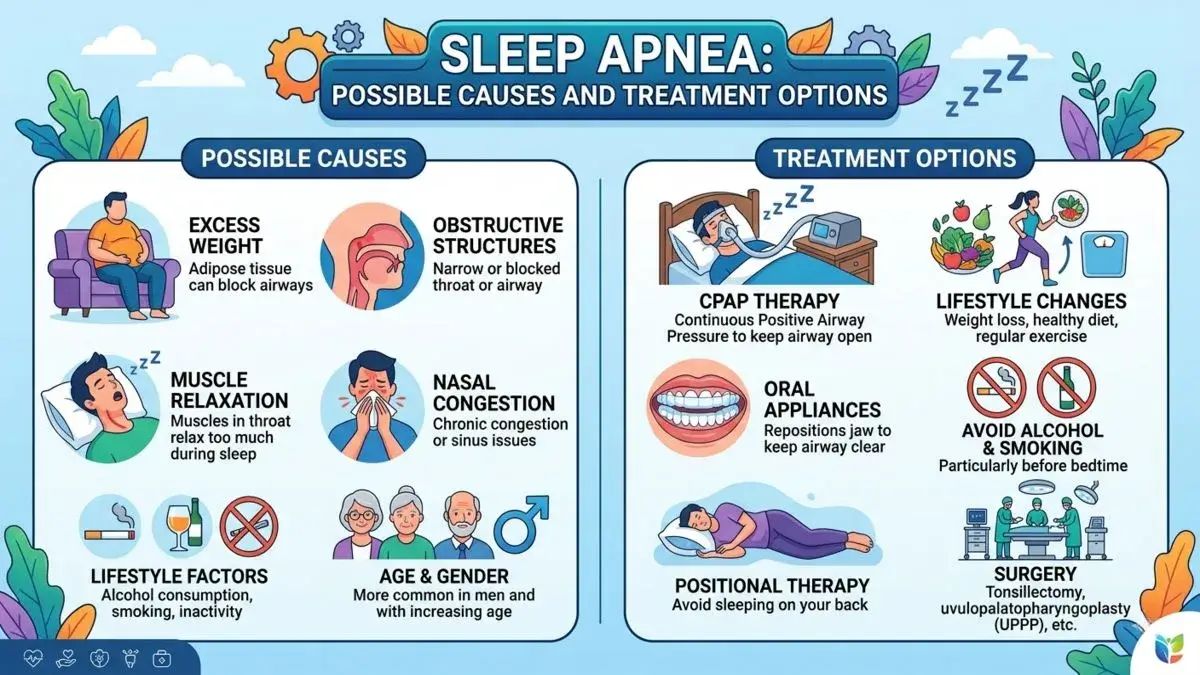
Sleep apnea is asleep-related breathing disorder where breathing repeatedly pauses or becomes shallow during sleep. These pauses may reduce sleep quality and cause symptoms such as loud snoring, choking or gasping during sleep, morning headaches, daytime tiredness, and difficulty concentrating.
Some people may not realize they have sleep apnea until a bed partner notice pauses in breathing or loud snoring. Medical assessment may help determine the type and severity of sleep apnea and guide suitable treatment options.
Table of Contents
What Is Sleep Apnea?
Sleep apnea occurs when normal breathing is interrupted during sleep. The most common type is obstructive sleep apnea, which happens when the upper airway becomes partially or fully blocked during sleep.
There are also other forms of sleep apnea, including central sleep apnea, where the brain does not send regular breathing signals during sleep. Some people may have mixed features. A sleep assessment may be needed to identify the type involved.
Common Signs and Symptoms of Sleep Apnea
Sleep apnea symptoms may occur during sleep or after waking. Common signs include:
- Loud or frequent snoring
- Pauses in breathing during sleep
- Choking, gasping, or snorting during sleep
- Restless sleep
- Waking with a dry mouth or sore throat
- Morning headaches
- Daytime sleepiness
- Difficulty concentrating
- Irritability or mood changes
- Reduced sleep quality
- Waking up feeling unrefreshed
Not everyone with sleep apnea snores, and not everyone who snores has sleep apnea. However, snoring with witnessed breathing pauses, choking episodes, or daytime tiredness may need medical review.
Possible Causes of Sleep Apnea
Sleep apnea can occur for several reasons. The cause may vary depending on the patient’s airway structure, sleep position, medical history, and lifestyle factors.
Narrowing or Collapse of the Upper Airway
In obstructive sleep apnea, the airway may narrow or collapse during sleep. This can happen when the muscles around the throat relax, reducing airflow.
Airway narrowing may involve the soft palate, tongue base, tonsils, nasal passages, or throat structures.
Nasal Blockage
Nasal obstruction can contribute to mouth breathing and disturbed sleep. Causes may include allergic rhinitis, sinusitis, nasal polyps, enlarged turbinates, or a deviated nasal septum.
An ENT specialist may assess whether nasal blockage is contributing to snoring or sleep-related breathing symptoms.
Enlarged Tonsils or Adenoids
Enlarged tonsils and adenoids may narrow the airway, especially in children. This may lead to loud snoring, mouth breathing, restless sleep, and pauses in breathing during sleep.
In adults, enlarged tonsils may also contribute to airway narrowing.
Weight-Related Factors
Excess weight may increase tissue around the neck and upper airway, which can narrow the breathing passage during sleep. Weight-related factors may also increase the likelihood of snoring and obstructive sleep apnea.
Jaw, Tongue, or Facial Structure
Some people may have airway narrowing due to jaw position, tongue size, or facial anatomy. A smaller lower jaw, recessed jaw, or larger tongue may contribute to obstruction during sleep.
Ageing and Muscle Tone
As people age, the muscles in the throat may lose tone. This can increase the chance of airway narrowing during sleep.
Alcohol, Sedatives, and Smoking
Alcohol and sedatives may relax the muscles of the throat and worsen airway collapse during sleep. Smoking may irritate the airway and contribute to inflammation or swelling.
Medical Conditions
Certain medical conditions may increase the risk of sleep apnea or worsen symptoms. These may include nasal allergies, thyroid disorders, heart conditions, neurological conditions, and metabolic disorders.
How Sleep Apnea May Be Assessed
Assessment usually begins with a review of symptoms, sleep history, medical history, and risk factors. The doctor may ask about snoring, witnessed breathing pauses, daytime sleepiness, sleep position, nasal symptoms, weight changes, and medication use.
An ENT doctor may examine the nose, throat, tonsils, tongue base, and upper airway. In some cases, a sleep study may be recommended to assess breathing patterns, oxygen levels, and sleep disruption.
Treatment Options for Sleep Apnea
Treatment depends on the type, severity, and possible causes of sleep apnea. Management may include lifestyle measures, breathing devices, oral appliances, treatment of nasal or throat conditions, or surgery in selected cases.
Lifestyle Measures
Lifestyle changes may help reduce symptoms in some patients. These may include:
- Weight management where relevant
- Avoiding alcohol close to bedtime
- Avoiding sedatives unless medically necessary
- Sleeping on the side instead of the back
- Maintaining a regular sleep routine
- Stopping smoking where applicable
Lifestyle measures may be used alone in mild cases or alongside other treatment options.
Continuous Positive Airway Pressure Therapy
Continuous positive airway pressure therapy, commonly known as CPAP, uses a machine that delivers air pressure through a mask during sleep. This helps keep the airway open.
CPAP is commonly used for obstructive sleep apnea, especially when symptoms are moderate or severe. Some patients may need time to adjust to the mask and pressure settings.
Oral Appliances
Oral appliances are dental devices worn during sleep. They may help reposition the lower jaw or tongue to reduce airway narrowing.
These may be considered for some patients with mild to moderate obstructive sleep apnea or for those who cannot tolerate CPAP. Suitability depends on dental health, jaw structure, and sleep study findings.
Treatment for Nasal Conditions
If nasal blockage contributes to poor sleep or CPAP difficulty, treatment may focus on conditions such as allergic rhinitis, sinusitis, nasal polyps, enlarged turbinates, or a deviated septum.
Treatment may include medication, allergy management, nasal sprays, or procedures where clinically appropriate.
Tonsil or Adenoid Treatment
For children with sleep apnea related to enlarged tonsils or adenoids, treatment may involve assessment of the upper airway. In selected cases, surgery to remove the tonsils or adenoids may be discussed.
In adults, tonsil-related airway narrowing may also be assessed as part of sleep apnea management.
Surgery for Airway Obstruction
Surgery may be considered in selected patients when a clear area of obstruction is identified or when other treatments are unsuitable or insufficient. Surgical options depend on the site of airway narrowing and may involve the nose, soft palate, tonsils, tongue base, or jaw.
Not every patient with sleep apnea is suitable for surgery. Assessment is needed to determine whether surgery may be appropriate.
Why Treatment Matters
Untreated sleep apnea may affect sleep quality, daytime alertness, concentration, mood, and work performance. In some patients, it may also be associated with other health concerns, especially when breathing interruptions and oxygen drops are significant.
Medical assessment can help identify the severity of the condition and guide management based on the patient’s symptoms and risk profile.
When Should You See an ENT Specialist?
You may consider consulting an ENT specialist if you experience:
- Loud or frequent snoring
- Witnessed pauses in breathing during sleep
- Choking or gasping during sleep
- Persistent daytime sleepiness
- Morning headaches
- Poor sleep quality
- Nasal blockage with snoring
- Mouth breathing during sleep
- Recurrent throat or tonsil symptoms
- Snoring or breathing pauses in a child
An ear, nose and throat specialist may assess whether nasal, throat, tonsil, or airway factors are contributing to sleep apnea symptoms.
-

 GENERAL11 months ago
GENERAL11 months agoChristofle – For Those Who Dream of Family Heirloom Silver
-

 SPORTS1 year ago
SPORTS1 year agoDiscover the World of Football with Streameast: Watch Your Favorite Leagues and Tournaments
-

 GENERAL4 months ago
GENERAL4 months agoUncovering the World of кинокрадко: The Dark Side of Film Piracy
-

 GENERAL2 months ago
GENERAL2 months agoATFBooru: Anime, Gaming, and Subculture Imageboard